Close menu
- Home
- Sectors
- Topics
- Local
- Comment
- Interactive
- Events
- Jobs
- Products & Services
- Subscribe
Expanded roles envisaged for non-medical staff
By Shaun Lintern2014-10-23T00:01:00
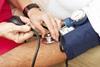
The roles and responsibilities of non-medical NHS staff would be dramatically expanded under the five year forward view
You need to be signed in to read more

Subscribe for unlimited access
With a HSJ subscription you’ll unlock:
- All of HSJ.co.uk and our HSJ mobile app
- News and insight on all areas of public funded healthcare
- Expert commentary, insight and analysis from industry leaders
- 9 weekly ‘Expert Briefing’ insight emails covering a variety of specialist topics
HSJ is part of Wilmington Healthcare Limited. Company number 2530185. c/o Wilmington plc, 5th Floor, 10 Whitechapel High Street, London E1 8QS. Registered in England and Wales. Company registration 30158470
Site powered by Webvision Cloud