Alan Turrell from Walsall CCG considers the merits of applying public value management theory to procurement in healthcare
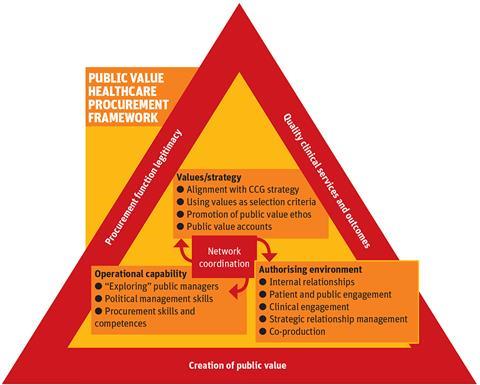
Public value healthcare procurement framework
Given the controversy and debate concerning the application of the procurement, patient choice and competition regulations, it is clear that whatever the interpretation there will inevitably be a greater focus on how formal procurement processes are conducted in the commissioning of NHS funded services. Clinical commissioning groups and their clinical support units will need to be turning their minds to what their approach to procurement should be.
A recent study has identified that there could be considerable merit in applying public value management theory, as originally proposed by business professor Mark Moore in 1995, to the procurement of healthcare and this will form the basis of the approach to healthcare procurement being adopted by Walsall CCG.
‘Public value considers the broader contribution of public services to society as a whole and is focused on meeting the needs of the public’
In the current context it is relevant to understand that public value theory emerged as an alternative to new public management, which centred on improving efficiency, meeting targets and treating individuals as consumers.
In contrast, public value considers the broader contribution of public services to society as a whole and is focused on meeting the needs of the public, as citizens as well as consumers, with creating value as the key driver rather than achieving targets.
As outlined below, five key themes relating to public value may be identified that are particularly relevant to the commissioning and procurement of healthcare.
Key public value theory themes
1. Strategic triangle:
- Public value can only be created if all three elements − strategic goals/values, the authorising environment and operational capability − are aligned as much as possible.
- This will inevitably require trade offs between these three elements and between competing values.
2. Emphasis on societal rather than individual needs:
- Combines “what the public most values” with “what adds value to the public sphere”.
- Deliberation required to determine public values/refined preferences.
- The achievement of public values must be measureable.
3. The role of public managers with emphasis on political management:
- Public mangers are “explorers and creators” of public value.
- Managerial view is outward, upward, downward and inward.
- A new role requires new skills and competences.
- Political management skills are a key competence.
- Experience, skills and knowledge of organisation constitute capital value.
4. Networked governance including mixed economy:
- Leadership across boundaries.
- Mixed economy.
- Management of network of providers.
5. Co-production:
- Co-production in both planning and service provision.
Applying these themes specifically to the procurement of healthcare in the form of a public value healthcare procurement framework (figure 1, below) gives considerable potential to address some of the key fears about the current choice and competition approach.
Central to this is Moore’s strategic triangle, which determines that the combination of the agreement of values and overall strategy, the approval of the authorising environment and the availability of the appropriate operational capacity are essential to any strategy aimed at the creation of public value.
Traditional procurement challenged
With its emphasis on societal goals, and the notion that public value extends “beyond market economic considerations”, the public value approach challenges traditional healthcare procurement whereby price and service quality criteria, rather than any broader societal goals, are the key considerations.
Taking the values/strategy sphere first, it is insufficient merely to align the procurement approach to the organisation’s values and strategy but it is essential that there is engagement in the overall strategic planning process so that procurement is leading not just following.
For example, at Walsall CCG the contracting and procurement function has played a key role in contributing to the CCG authorisation process and the development of the group’s integrated plan by demonstrating that there is a good understanding of the current provider landscape through the conduct of a spending analysis and that market management, strategic procurement and robust contract management are key components of the overall commissioning strategy.
‘Clinical and public engagement throughout all stages of the procurement process is vital’
This will be a particular challenge where CCGs have opted to contract out their procurement functions to CSUs. As the new commissioning organisations develop, first impressions will be key and the procurement approach will need to heed leadership expert Linda Holbeche’s warning that “too much bureaucracy at an early stage signals lack of trust and stifles innovation” and hence a more flexible approach to procurement will be required.
A crucial element here will be embedding NHS values into the procurement process, including their use as selection and evaluation criteria and the promotion and monitoring of the public value delivered by providers. This could take the form of requiring providers to publish “public value accounts” alongside their quality accounts.
Turning to the authorising environment, clinical and public engagement throughout all stages of the procurement process from specification development, tender evaluation and contract management, is vital. The role of the procurement function, whether internal or outsourced, will be critical here in developing a myriad of internal relationships that will be essential if procurement is to be seen as a critical strategic function.
Commissioning and procurement leaders will need to adopt Moore’s vision of public managers not only as “explorers” but as “moral leaders” whose “ethical responsibility is to undertake the search for public value conscientiously”. It is unlikely that procurement managers would currently describe their role in this way. However, if they adopted this as a blue print for the future it would go a long way to securing legitimacy within their new organisations, as well as putting the public value message firmly on the agenda.
In this sphere, dialogue with the provider base is also crucial. The adoption of strategic relationship management, widely used in the commercial sector, is advocated to maximise the public value delivered by key providers. This approach could be used to help reinforce a public service ethos and to measure the public value created. This is a far cry from the “let and forget” approach to awarding contracts sometimes encountered in the NHS.
Promote co-production
The promotion of co-production is also essential and this may operate in two ways. First, by awarding contracts specifically for the delivery of co-production activities; for example, selecting a provider to deliver an expert patient programme. Second, by awarding contracts that oblige providers to engage their clients in co-production activities.
‘The public value healthcare procurement framework puts the creation of public value for the benefit of the community as a whole at the centre’
Within operational capability, procurement skills and competences are top of the agenda, but these must be enhanced by incorporating Moore’s emphasis on political skills in building effective internal relationships, as well as gaining external political legitimacy. This approach is consistent with the findings of Lonsdale and Watson that conflict and power, rather than technical issues, are fundamental in determining effective internal customer relations in the NHS procurement process.
Where applicable skills and experience in procurement have been acquired it is important that they are regarded as being part of the “capital value” of the organisation and this may lead commissioning organisations to determine whether or not it is appropriate to outsource their contracting and procurement functions.
The intersection of the three spheres illustrates that a major role for the procurement function, and one that is perhaps not generally recognised in practice, is as a network coordinator. This involves: acting as the principal interface between the organisation and its external providers; coordinating, interpreting and consolidating the requirements of internal customers to avoid fragmentation of spending; and “steering networks of providers in the quest for public value creation”, as Professor Janine O’Flynn said.
New approach
Although some of these elements are already in place, the public value healthcare procurement framework as a whole represents a new approach that, as illustrated by the outer triangle, puts the creation of public value for the benefit of the community as a whole at the centre of healthcare procurement. In doing so it promotes increased legitimacy of the procurement function and strengthens the delivery of clinical outcomes.
This approach is also consistent with the recently enacted Public Services (Social Value) Act 2012, which requires all public bodies, including CCGs, to consider: “How what is proposed to be procured might improve the economic, social and environmental wellbeing of the relevant area.” Further, “How, in conducting the process of procurement, it might act with a view to securing that improvement.” Adhering to this requirement in itself may go a long way to tempering some of the fears about the impact of increased tendering of healthcare services.
By combining this with a public value approach that promotes a public service ethos among all providers, adopts public values as evaluation criteria, focuses on the measurement of the public value delivered by providers, and encourages the use of co-production is likely to contribute to what former Labour MP David Marquand calls the “humanisation” of private provision.
All these ingredients are part of the procurement strategy being developed by Walsall CCG and we are discussing this approach with public and patient representatives and with third sector organisations. The CCG chair, Dr Amrik Gill, has already found that: “By emphasising that our approach is focused around social values and on creating public value, it helps to reduce some of the fears about the impact of increased competitive tendering and greater public provision”.
The adoption of a public value approach to the procurement of healthcare shows that increased tendering and procurement activity may not necessarily undermine NHS values, but may actually serve as a sound instrument in promoting and preserving them.
Alan Turrell is head of contracting and procurement at Walsall CCG


























No comments yet