Input growth rate is down and overall growth projections fall far short of levels required by the NHS Five Year Forward View
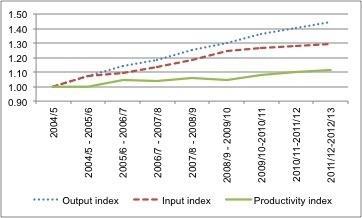
As the latest Centre for Health Economics report shows, the NHS has delivered positive productivity growth of 10.4 per cent over the nine years from 2004-05 to 2012-13.
It also reveals that the NHS achieved a third consecutive period of year on year productivity growth between 2011-12 and 2012-13 (the latest year for which national data is available).
That sounds like a good reason to crack open the champagne, but there are some sobering facts behind the figures.
‘Recent productivity growth is mainly the result of a low rate of input growth’
First, recent productivity growth is mainly the result of a low rate of input growth.
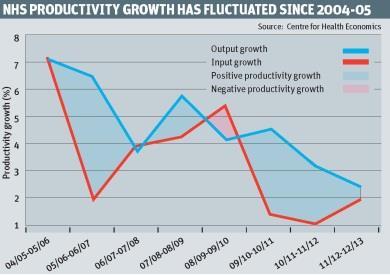
While output growth was 2.34 per cent between 2011-12 and 2012-13, inputs grew by just 1.98 per cent, leading to positive productivity growth of 0.36 per cent.
The input growth rate of 1.98 per cent is considerably lower than the average year on year input growth of 4.53 per cent between 2004-05 and 2009-10, but the highest since the coalition came to power – the growth rate was 1.33 per cent between 2009-10 and 2010-11 and just 1 per cent between 2010-11 and 2011-12.
- Charlesworth, Murray: Current NHS support is not enough, we need a transformation fund
- West: Politicians seek to distract from the funding question
- Hopson: We can’t just ‘do the same again’ to make £22bn of NHS efficiencies
Labour pains
The low rates of input growth have been achieved by restraining growth in labour inputs, which account for around half of total inputs.
NHS staffing input actually fell by 0.24 per cent between 2010-11 and 2011-12, and by 1.95 per cent between 2011-12 and 2012-13.
‘NHS staffing input actually fell by 1.95 per cent between 2011-12 and 2012-13’
These later reductions were concentrated among nursing, midwifery and health visiting staff (3.7 per cent fewer), scientific, therapeutic and technical staff (2.6 per cent fewer), and administrative and estates staff (3 per cent fewer).
Reductions in NHS staffing input between 2011-12 and 2012-13 were more than offset by increases in the use of intermediate inputs (such as supplies and services, establishment, and external purchasing), capital and agency staff. This led to positive total input growth.
Further reductions in NHS staffing input are unlikely, as staffing levels have increased following the November 2013 recommendations of the Francis inquiry.
The Health Foundation captures this in its recent study, Hospital Finances and Productivity: In a Critical Condition?, which suggests that hospital productivity fell by 1 per cent between 2012-13 and 2013-14.
Given that hospitals account for about half of the NHS, their poor productivity performance will pull down the figures for the NHS as a whole when these become available.
Slower output
Second, output growth has slowed. The annual growth rate of 2.34 per cent for 2012-13 is the lowest year on year since 2004-05, and well below the average of 4.65 per cent.
This low growth reflects a recent slowdown in activity growth, and deteriorations in quality, with slight reductions in survival rates for non-elective patients and further increases in waiting times.
The NHS may not quickly return to higher rates of output growth: although quality is not considered in its analysis of hospital productivity, the Health Foundation reports lower annual increases in accident and emergency visits, outpatient attendances and inpatient admissions in 2013-14 than for previous years.
Off target
Third, although year on year productivity growth has averaged 1.26 per cent since 2004-05, this is a long way short of the 2-3 per cent required in the forward view to help close a funding gap that is otherwise projected to widened to £30bn by 2021.
With population growth of 0.6 per cent a year and people living longer with multiple chronic conditions, pressures on the NHS are not going to ease.
‘320,000 fewer people received local authority supported social care in 2012-13’
The health service also has to cope with reductions in social care funding – around 320,000 fewer people received local authority supported social care in 2012-13 than in 2005-06, despite the number in need increasing.
It will not be possible to meet these demand pressures without extra financial support. All political parties have recognised this but extra funding will be conditional on the NHS delivering further productivity gains.
An approach that focuses exclusively on short term adjustment to labour inputs, whether through permanent or agency staff, will not generate long term performance improvements.
Instead, the more strategic vision set out in the forward view is required - involving changes to the existing configuration of services, improvements to urgent and emergency care, and greater emphasis on prevention and public health.
Andrew Street is professor of health economics and director of health policy for the University of York’s Centre for Health Economics



























4 Readers' comments