NHS App director reverses decision to join tech consultancy firm
The national director for NHS digital channels has reversed his decision to join a tech consultancy firm as an advisor after the initital announcement was greeted with widespread criticism.
NHSE tells ICBs to slow elective referrals
NHS England has told integrated care boards they need to slow down elective referrals dramatically – nearly eliminating year-on-year growth – with high-profile waiting list targets under threat.
Revealed: The systems set to gain and lose hundreds of millions
Nine integrated care systems are set to lose hundreds of millions in NHS funding relative to others in coming years – while eight stand to make big gains – under new NHS England funding policy.
NHSE commends ICBs for ‘strong leadership’
The quality of leadership at 13 integrated care boards has been praised by NHS England in its latest formal assessment of their performance.
Tariff ‘insufficient’ for ‘premium’ cost of tackling long waiters, warns CEO
There is “insufficient” funding for extra work needed to tackle long waits, a chief executive at one of the worst-performing trusts against a key elective target has said.
ICB chair steps down to join double-merger trust
An integrated care board chair is leaving her role to join an integrated trust in the West Country, it has been announced.
Trust in financial dispute with two ICBs
An ambulance trust has warned it may miss financial targets because it has failed to finalise some commissioning contracts halfway through the year.
Three ICSs responsible for a quarter of very long diagnostic waits
Just three integrated care systems were responsible for nearly one in four 13-week waits for key diagnostic tests in recent months, HSJ analysis of official data has found.
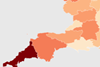
Revealed: Three-fold variation in emergency response time by ICS
A threefold variation in ambulance response for serious, urgent conditions has been revealed in new figures.
ICB admits defeat on key September target
An East of England integrated care board expects to miss both the main national elective recovery target of eliminating 65-week breaches by September and a top diagnostic target, according to board papers.
Threefold ICS variation in GP phone access revealed
Patients trying to reach their GP are almost three times as likely to fail to get through in the worst-performing integrated care systems than the best, according to analysis of new annual figures.
The Integrator: The ‘race to the bottom’ in ICS finances
Insider tales and must-read analysis on how integration is reshaping health and care systems, NHS providers, primary care, and commissioning. This week by deputy editor Dave West.
‘Patients are choosing palliative care over cancer treatment’ due to lack of local services, CEO warns
Patients in part of the East of England are choosing to begin palliative care over cancer treatment because of prohibitive travel times and costs to get to the nearest specialist centre, a local system leader has warned.
ICB hires overseas CEO for new £1.5bn commissioning job
An integrated care board has brought in a senior executive from overseas to lead the commissioning of £1.5bn worth of delegated specialised services for the East of England.
Trust ‘fighting losing battle’ over elective waits, CEO admits
A hospital chief executive has blamed a “mind-blowing increase” in cancer referrals for his trust’s deterioration in performance on long elective waits.
Strikes spread to more trusts over backpay dispute
Strike action by healthcare assistants looks set to spread to more trusts, having so far been confined to the North West region.
Nearly a third of ICSs admit finance plans will be missed
At least 13 integrated care systems have now admitted they will miss the financial plans they signed up for at the start of the year.
London gets well over ‘fair share’ of specialised services while rural areas miss out
People in some more rural areas are missing out on specialist treatments they should be getting, while Londoners are receiving a lot more than their “fair share”, new NHS England figures suggest.
Exclusive: Government and NHS in talks over £1bn funding gap
Government is in talks with national NHS leaders over how to fill an urgent funding gap of at least £1bn this financial year, HSJ has learned, as new analysis shows all 42 local integrated care systems were behind their own plans less than halfway through 2023-24.
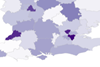
Revealed: First ICS digital maturity ratings
HSJ can reveal the first ratings given to every integrated care system for the ‘digital maturity’ of its NHS providers.