For obese patients with osteoarthritis in their knees, surgery often leads to further weight gain. Henning Bliddal argues that changing behaviour and reducing the body weight can work wonders and save the NHS money
Around 60,000 British patients face the trauma of knee surgery each year, and hundreds of clinical commissioning group and Scottish Health Board managers have to pay for it.
‘The best time for adopting healthier lifestyle and learning new behaviour is before surgery, not after’
The obesity epidemic is compounding the problem.
Obesity is a risk factor for osteoarthritis – it increases symptoms and makes it more difficult to exercise.
Yet this cycle of distress – involving anguish all round and millions of pounds of taxpayers’ money – can often be prevented.
- Moving with the times: a preventative approach to musculoskeletal health
- Morbidly obese patients face restrictions under new Devon cost cutting plan
- Roundtable: Put nutrition at the centre of public health
- Obesity evidence: There are diets as effective as the knife
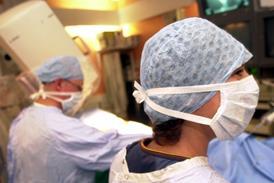
Surgery isn’t always the answer
I was sceptical when my team set out on a journey to reduce the numbers of patients referred for knee surgery five years ago. Now, in all obese patients with osteoarthritis, rapid weight loss of around 10 per cent of body weight should be a first line management approach.

But since even surgeons are adjusting to this news, I had better explain.
I am proud of our international reputation at the Parker Institute in Copenhagen, but even we were wedded to convention. And convention says – or, rather, it used to – that, if someone has osteoarthritis of the knee, the only definitive solution is surgery, and a new joint.
Because if you give obese patients a new knee, they will become more active, exercise and lose weight. Right?
Wrong.
‘After surgery, obese patients actually put on more weight’
It is quite the reverse. This group actually puts on even more weight, as evidenced by a large cohort study in US – probably because the reduction of pain after the operation means they forget to hold back and return to overeating.
So they put even more strain on their precious new joint knee, increasing risk of wear. In the end, they need a replacement joint – a nightmare for patients and causing hefty surgery costs.
The best time for adopting healthier lifestyle, learning new behaviour, and reducing calories and weight is definitely before surgery, not after.
Vicious cycle
Today, 10-15 per cent of Danish adults are obese. In Britain, it is 25 per cent.
When people put on weight, their knees suffer from all kinds of trouble including pain caused by inflammation. The result is that they become less active and give up exercise, producing a downward spiral. Many patients become housebound.
‘When people put on weight, their knees suffer from all kinds of trouble, including pain caused by inflammation’
This is a source of pain that affects millions of Britons, yet just a 10 per cent reduction in body weight will have a substantial impact on the lives of this group.
But if someone cannot exercise, how can they possibly lose the weight?
To find out, we teamed up with Arne Astrup, head of the department of nutrition, exercise and sports at the University of Copenhagen, and a specialist in meal replacement low calorie diets which comprise of soups, shakes and bars.
No Danish weight loss companies were prepared to back us, but the Cambridge Weight Plan, led by Anthony Leeds, was.
Calorie count
We selected 192 typical patients, who were elderly and had knee problems that prevented exercise. Some could not even get onto our 12m catwalk for initial biomechanical assessments.
They all received either a low calorie (810 calories per day) or very low calorie (between 415 and 540 calories per day) liquid formula diet for eight weeks, followed by a 1,200 calorie daily diet for a further eight weeks. They were then randomised into one of three groups for maintenance for the subsequent year.
Patients found rapid weight loss was motivational and successful. And we identified for the first time the improvement in pain and function that can be achieved with weight loss.
‘A 10 per cent weight loss produced a 30 per cent improvement in quality of life’
A 10 per cent weight loss produced a 30 per cent improvement in quality of life. Because this 30 per cent alleviated some of their worst issues, the impact on quality of life was all the more significant.
From being house bound, some could soon do many things we all take for granted: walk, climb stairs, visit friends and grandchildren, and go shopping. One patient literally walked again.
Lives were truly transformed.
We have also shown, for the first time, that weight loss through a low calorie diet can be maintained for four years, with all the associated health benefits such as a reduction of blood pressure, thereby reducing their overall cardiovascular risk and creating further savings on drugs.
Their nutrition was improved throughout. And improvements in their vitamin D status may have helped to maintain vital bone minerals and density.
And not a scalpel in sight.
Truly transformative
These findings have huge implications as our populations age and obesity snowballs.
Thus, all heavyweight people should be offered intensive weight loss before considering joint replacement. Even if it comes to surgery, their lighter weight will reduce the risk of complications such as infection, and will ease rehabilitation.
‘Once they have experienced a profound increase in quality of their life, most of them stick with the programme for years’
If we just lean back and wait for the surgeon, society is facing problems of unknown dimensions.
But whom must we persuade to act? Politicians, surgeons, CCGs or health and wellbeing boards? Well, all of them – but, from our experience, certainly not patients.
Once they have experienced a profound increase in quality of life, most of them stick with the programme for years. They are 100 per cent on side, and surely, they must come first.
Henning Bliddal is head of the Parker Institute in Copenhagen

























1 Readers' comment