NHS commissioners could save more than £800m over the next decade by improving care pathways for patients with chronic obstructive pulmonary disease, analysis available exclusively to HSJ subscribers suggests.
The analysis by health information specialists Sg2 projects how much COPD patients will cost NHS commissioners in each primary care trust area by 2020. It then sets out for each primary care trust the savings possible through better managing the COPD pathway.
The data is timely as COPD exacerbations are common over winter months, creating capacity issues at hospital providers.
The disease accounts for one in eight emergency admissions in the UK and the second highest number of bed days.
The data suggests PCTs could save an average of £5.3m each by 2020 if they implemented programmes to educate patients and help them manage their condition without the need for hospital stays or going to accident and emergency. That could reduce the number of COPD hospital spells by an average of 33 per cent by 2014.
The potential savings were calculated by multiplying the number of spells the research predicts could be avoided by the relevant tariff price, adjusted for market force factors.
Researchers found most potential for savings in parts of the North West, North East and Yorkshire and the Humber, where rates of COPD are high.
With an estimated saving of £3,621 per 1,000 of the population, NHS Knowsley was found to have the biggest potential.
NHS Barking and Dagenham was identified as having the greatest potential for reducing hospital stays, with researchers predicting those could be cut by 41 per cent from 319 spells in 2008-09 to 216 in 2014. Six of the 10 PCTs with the biggest potential for reducing hospital stays were also in London.
NHS Knowsley medical director Chris Mimnagh told HSJ the PCT had introduced many of the actions suggested by Sg2 through a COPD service run by St Helen’s and Knowsley Teaching Hospitals Trust, which had an annual cost of £1.2m.
The service includes a 24/7 helpline, patient action plans and community based clinics staffed by consultants and a dedicated team of COPD nurses.
Dr Mimnagh said: “It’s still early days but it’s showing a drop in A&E attendance and admissions. We are moving in the right direction.”
In 2009-10 the PCT saw 690 fewer A&E attendances, 145 fewer emergency admissions, and 58 fewer emergency readmissions than in 2008-09.
The data
- See the results for your PCT area here, along with in-depth analysis and information on how to create savings in your organisation: www.hsj.co.uk/5021475.article
COPD care: how to save millions
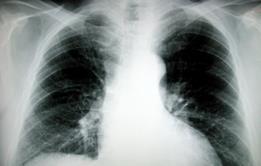
With seasonal capacity issues rising, this quarter’s HSJ Change Forecast focuses on COPD and explores how a proactive approach to care pathway management could save over £800m on COPD inpatient care alone.
- 1
 Currently
reading
Currently
reading
£800m savings identified through better COPD care
- 3
- 4




























5 Readers' comments