Dementia research revealed how better planning and a reduction in medication can improve quality of life and make big savings, say Julia Oxenbury and colleagues.
The government’s dementia strategy aims to improve the quality of care across three areas: improved awareness, earlier diagnosis and intervention, and higher quality of care. At the South West Peninsula deanery we found two key aspects that can easily improve treatment:
- better planning for advanced care of patients with dementia helps improve quality of life for patients and families;
- reducing levels of medication actually improves patient health and leads to sharp reductions in the number of unplanned secondary admissions.
The need for improved care for people with dementia led to a desire within our deanery to make changes at a local level. We were fortunate in having a resource on hand: within the deanery, a number of general practice trainees were appointed for an additional fourth year. One of these ST4 trainees was tasked with researching advanced care planning in care homes across Cornwall to determine whether improved care planning could reduce unplanned hospital admissions.
The ST4 trainee also began to collaborate with the clinical nurse specialist for dementia in Cornwall and Isles of Scilly Primary Care Trust who had been developing her own training programme for nursing homes, focusing on care planning.
The research found that prevailing standards were low. Although the Mental Capacity Act of 2005 declared it against the law to treat older people and those who are infirm against their wishes and against the wishes of their families, this regulation has been widely ignored in practice.
The initiative aimed to train nursing home staff to complete advanced care planning for patients with diminished capacity. Staff and relatives were then encouraged to meet to complete a best interest document, with the ST4 trainee on hand if there were any queries.
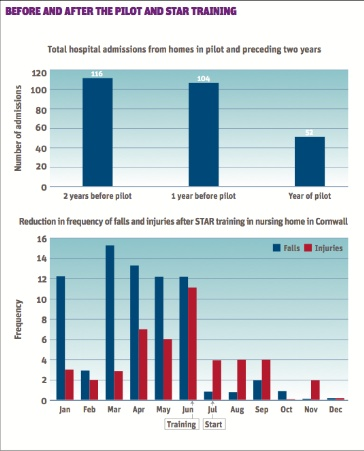
The initial results were very promising. In the area covered by the projects there has been a 50 per cent reduction in unplanned admissions (‘Before and after the pilot and star training’ graph) and, in accordance with the wishes of the families, all deaths recorded occurred in nursing homes rather than in hospital.
As the cost of an unplanned hospital admission for a person with dementia is approximately £2,000, we estimate the cost saving - over the course of 12 months - to be approximately £100,000. The financial implications of this project are vast, but the implications for carers and families are profound also.
It has been known for some time that over-medication is prevalent among patients with dementia in nursing homes. Cornwall and Isles of Scilly PCT aimed to address this by developing a training programme based on STAR (stop, think, assess, review) methodology to enable nursing home staff to identify ways of reducing major and minor tranquilliser use.
In the main, nursing home staff were extremely receptive and embraced the training programme. It was observed that patients on reduced medication became more alert and more responsive, were able to eat and drink independently, enjoyed more sleep and were less prone to hallucinations. The table (below) shows some of the behavioural improvements that were observed with a selection of our sample of 12 patients.

Significant numbers
The result was a net gain all around. The patients enjoyed better health, nursing staff did not have to deal with so many “difficult” patients and the cost savings were staggering. The savings for the 12 patients in the sample alone amounted to £105.25 per month, equating to £1,263 per year or approximately £100 per patient per year. Multiply this by the number of people across the UK who have dementia and the number becomes very significant indeed.
After delivering STAR training, the researchers followed up on the numbers of falls and injuries reported by nursing homes. The number of falls and injuries reported at a single nursing home in Cornwall are detailed (see graph opposite); prior to STAR training, this home was reporting an average of around 11 falls and six injuries per month.
The decline in falls and injuries after STAR training was dramatic - dwindling to zero on both counts by December. Once again, the real improvement in the quality of patients’ lives was accompanied by considerable resource savings and an associated reduction in unplanned hospital admissions.
It has already been established that general practice training programmes should be four years. This project has highlighted the added value that an additional year of training provides, not only for the doctor but also for the community and the public purse.
We are planning to expand the advanced care planning and medication review programmes into nursing homes in Devon.
It is hard to stress the importance of these findings. Dementia is a serious national issue and dementia care has been demonstrated to be failing on many levels. We found that advanced care plans, coupled with relevant medication and treatment, result in a quality of life for patients that is much improved, and happier, more involved families. Furthermore, substantial savings are made in relation to costs as well as medication and secondary care resources.
We have also shown how general practice trainees can make a real difference to people’s lives and that cross-boundary initiatives within the NHS can produce significant synergies.
This project pushes all the right buttons. We believe more initiatives like this are needed, not just in the South West but across the NHS.
Julia Oxenbury is a GP dean at the South West Peninsula deanery. Paula Marrett is a GP ST4 trainee at Fowey River Practice, Cornwall. Bev Chapman is a clinical nurse specialist in dementia at Cornwall and Isles of Scilly Primary Care Trust.























No comments yet