We asked readers what behaviour and process changes do they believe are needed for the NHS to deliver consistent, financially sustainable 24/7 working. These are the most popular answers regarding care delivery
The NHS cannot provide 24/7 working with social care providing the same
It is right that patients have a consultant-led service on a Saturday with a full complement of radiographers, pharmacists occupational therapists and so on. However what is the point if the frail 87-year-old has their discharge delayed as a package of care cannot be started until Monday?
I believe the question we are being asked is wrong. It should be: “What are the behaviour and process changes you believe are needed for health and social care to deliver consistent, financially sustainable 24/7 working?”
Bringing the NHS to 24/7 working without social care doing the same is akin to attempting to take a bold step forward only to realise that it it tied to the other and falling. We need a co-ordinated “hop”.
Care delivering over 24/7 is not an option
We need to move away from the idea that paeople become unwell only between Monday and Friday. Senior clinicians need to be available 24/7 to enable pathways of care to be delivered. At the present time we have a culture of no discharges after midday on Friday and no admissions until midday on Monday.
We need a robust social care structure that does not allow patient to languish in hospital beds as there are unable to go home and adequately funded community teams.
GPs need to offer extended hours and weekends.
NHS lastminute.com
A clearing system for unused capacity, outpatient, GP and inpatient capacity.
Currently, people use the appointments line and choose and book. Both are a bit crap, and work intensive for patients.
Instead, why not allow patients to be proactively contacted with appointment cancellations in their area or category. Let’s say I need a first outpatient appointment for whatever. I go onto a booking system (successor of C&B) and book, but at the same time, I am prompted to say I am interested in cancellations within 50 miles (I choose 50, because I’m mobile), and at a minimum of three days notice (because I’m flexible) for this specialty.
When something comes up, I’m notified by SMS or email, and asked if I can take the appointment, a bit like a proactive lastminute.com. That way, I don’t have to keep on phoning or checking randomly. That makes the thing cheaper, easier and it’s all existing technology that wouldn’t take a massive change.
New approaches to acute management of nursing home residents
Patients from nursing homes are frequently admitted through the medical take (via A&E) where a staff member has called an ambulance because of problems such as fall (described as collapse), worsening confusion and infections (frequently chest/urine).
It is difficult to assess these patients in the acute setting because there is generally no information about baseline level of function. Therefore a patient who is confused or cannot walk undergoes a full acute confusion screen/“collapse query cause” screen which often includes a CT brain.
However, the patient may already be bed bound and be known to have dementia and may not be much different from their normal baseline. Because of the four hour wait target, the patient is admitted as a default because background information cannot be obtained quickly enough. The patient then languishes on a general medical ward and is difficult to discharge. Suggest:
- Clinical passports for such patients with baseline functional information - hospital doctors need to know what to aim for from the outset.
- Better description of reason for ambulance being called - yes, they have had a collapse or are confused but did they just trip and fall over? How much worse is the confusion? Did they hit their head?
- Basic medical mangement of nursing home residents in nursing home - fluids and antibiotics in the nursing home early especially if ceiling of care is not for ITU/HDU.
- GP or other skilled professional assessment of patient before ambulance called. Better parameters for less skilled staff to follow to know when and when not to call an ambulance.
- Geriatrician outreach from secondary care to educate and to trouble shoot where there is high referral into hospital rates.
Personal responsibility and preventative health
Embrace technology and enable people to care more for themselves at home, especially those with long term conditions to manage.
Encourage self care and self management. Increase the focus on preventative health to help sustainability in the future. We need a mind set change so that people know they are responsible for managing their own health and for looking after themselves.
Move from “what can the NHS do for me?” to “how can I improve my own health and wellbeing?”
This won’t be easy but it’s not impossible
To deliver a true 24/7 service to patients we need:
- To keep the politics and politians out of these services - they need time to evolve, become sustainble and deliver. Chopping and chaning things every four years does nothing but waste money, lose corporate memory and feed disengagement and poor quality.
- To invest in the right things at the right time.
- To fully understand what services are needed, when, where they are needed and to be delivered by whom.
- A joined up health and social care service, so we stop fighting over the same “pound” and work together in the best interests of the patient – when they are medically fit to leave acute care their onward care should be quickly arranged and efficiently managed.
- Consultants/specialist nurses working in the community, visiting patients at home or in nursing/residential homes, if that affords the right care in their own setting.
- A single nursing structure to cover both acute and community needs with enough staff for 24/7 cover, fully skilled and trained to keep patients out of hospital if they can be treated at home, but able to expedicate an admission if needed (with the support of consultants also working in the community) without the need for an A+E attendance.
- All staff, including consultants, GPs and managers to move to a shift pattern of working that covers 24/7 and do away with unsocial hour premiums and the idea of being on-call.
- Adequate level of senior managerial presence in place 24/7.
- An acceptance that the same level of care, attention and availablity of service is needed 24/7, this would even out peaks and troughs if the population knew they could access service 24/7, including GPs.
Is it 24/7 or is it safe or can it be both?
This may be a stupid post, for which I apologise…..
Imagine if the week was just seven days, and there wasn’t a weekend. We still have a five day week and two days rest, but this can be at the beginning, middle or end, it doesn’t matter. Whatever we do is “on” one way or another. What a lot of waste there would be. 24/7 anything would be unaffordable.
I’m a clinician/ manager in my 40s and I remember early closing time on a Wednesday in the High Street. You managed around it. But health doesn’t fit into convenient slots. I don’t choose to have my MI on a Tuesday at 10am. And no software is sophisticated enough to predict that. Plus I might be run over by a bus at 9am instead. We can get terribly sophisticated about modelling and working out this that and the other, but what is more important is having safe staffing levels. If we have a major incident on a Sunday evening, we should be able to respond as well as if it were a Thursday. This debate should not be about making people feel guilty about their A4C increments or arguing with staff side about rotas, it should be a clinically led discussion with ALL the professions about what staffing levels are needed to run a safe service. And that means integration.
I struggle to explain 111 and OOH and WICs and MAUs and ED etc to family members, it must be even worse to navigate when you’re ill or scared or old or foreign or all of those. The whole health system needs to merge to form its own triage, and it should begin in the home and the community, not an ambulance or a hospital. This is more than just 24/7, this is rethinking the entire structure of health and social care, not the organisational musical chairs we’ve wasted the last decade or so on.
Topics
The wisdom of crowds: your views on 24/7 working
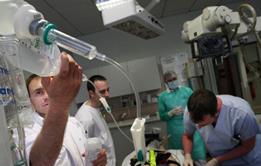
We asked for readers’ opinions on making 24/7 working successful
- 1
- 2
 Currently
reading
Currently
reading
Care delivery: your top ideas
- 4
- 5
- 6
- 7
- 8
- 9
- 10
- 11









































No comments yet