Mark Tooley and Bernie Marden analyse the impact on parents, children and staff of an innovative neonatal intensive care unit at their hospital in Bath

Baby
In 2007, the Royal United Hospital Bath decided to build a new £6.4m neonatal intensive care unit, half funded by the NHS and half funded by public donations, as the old unit was cramped, inefficient, dark and stressful for all the users.
The Forever Friends fundraising team led the public appeal, and the major donor for the project was the James Dyson Foundation. The Dyson Centre for Neonatal Care opened in July 2011.
The unique funding stream made it possible to challenge assumptions about what would be appropriate and possible. It was pivotal that new building promoted holistic healing, was focused on family centred care and was environmentally sustainable.

There is excellent natural light availability but, importantly for our vulnerable babies, this is extremely controllable. A quiet and calm environment was needed that would soften the stress of having a sick baby in this highly technological setting. The textured bare wood finish and controllable natural light is helpful in this regard.


A research team was established to measure the effects of the new facility on staff, parents, babies and the environment. The research measured how the existing unit had an impact on its users, and then after a period of adjustment in the new unit the measurements were repeated. A comprehensive data set was captured for both. We wanted to answer some questions such as:
- Is the quality of the environment in the new building demonstrably different to the old unit?
- Do parents in the new facility feel different and behave differently compared to parents in the old one?
- Do the staff feel different in the new centre?
- Is it possible to measure the impact of the new environment on babies?
More than 40 staff in the old unit and 40 in the new unit were studied, along with 10 families in each of the units.
To obtain a measure of the babies’ sleep and “settled-ness” we designed our own baby movement detectors. To gain an insight into the behaviour of the staff in the old and new units, the movement of all nursing staff was tracked continuously. This involved nurses wearing special tags containing wi-fi and infrared receivers. The sound and light in the buildings were measured by using commercial sound and light meters.
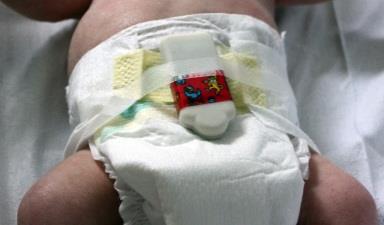
The baby movement detector is a small self-contained wireless device mounted on the babies nappy and measures their breathing, restlessness and sleep pattern. The low power and wireless specification is important as the device must not emit any heat or disturb the child.
The nurses would be located by wi-fi triangulation, and also their tag would pick up clinical location information by receiving the infrared beacons. Their location information was recorded continuously, throughout the 24 hour cycle, and then used to calculate the time spent in clinical rooms, caring for babies, and in non-clinical rooms, such as the nurses’ station and the coffee and milk rooms. The nurses were recorded anonymously and their locations could be viewed remotely online.
Findings
Parents reported that they felt less cramped in the new centre compared with the old unit, and they had less interference from noise and light. They felt less in the way and mothers felt more comfortable breastfeeding. In the new unit 90 per cent of the babies went home breastfeeding, compared with 64 per cent of children born in the old centre.
‘Initial results show that in daytime nurses spend, on average, nearly twice as much time in clinical rooms looking after the babies in the new unit’
In the old unit, we found mothers became more anxious the longer they stayed in, whereas in the new facility they felt more relaxed the longer they stayed. The same was true for fathers, though the impact was not so pronounced. We found parents visited their children more on the new unit, on average 30 minutes more a day, and when parents visited they spent more time in direct contact with their babies.
It was reported that babies in our cohort had 20 per cent more sleep on the new unit. Overall, it was 8 decibels quieter than the old centre, except for the period between 8am and 11am, when on average then it reached the same level as the old unit − but in some rooms, in particular the special care unit, the sound levels during 8am-11am were 6 decibels more.
The nurse tracking data obtained is immense, and still in the early stages of analysis, but initial results show that in daytime nurses spend, on average, nearly twice as much time in clinical rooms looking after the babies in the new unit as in the old one. Night time behaviour was similar in both, although still more time was given to care in the new facility.
Impact on care
Finally, the energy use in the old building was £80 per 100 cubic metre, compared wiht £50 per 100 cubic metre in the new unit, but the space in the new unit was nearly three times as much: 45 square metres increased to 121 square metres in the new unit.
‘This project clearly shows that building estates according to the needs of the patients improves quality of care’
In summary, the new unit is quieter, has more available and controllable light and is more energy efficient. The staff spend more time in clinical rooms, and parent and baby interaction has increased.
However, it was found that sound levels increase at certain times and we think that that is related to staff behaviour. This needs to be corrected for the building to be even more efficient. The baby detectors also suggest this extra sound has a negative effect on the babies sleep quality. We would also like to increase the amount of time parents visit throughout the 24 hour period.
This project clearly shows that building estates according to the needs of the patients improves quality of care.
Learning points from the project
- When planning to do a project like this, comparing an old and new building, it is wise to start the whole process well before the old building closes. Ethics, fund raising and recruitment of a team all take time. In this project, we only just finished the old building in time.
- Nurses needed time to get used to the tracking devices.
- Devices for babies had to be colours other than white, so they could be spotted if they were thrown away with nappies.
- The wi-fi in the smaller old unit was much easier to control than large hospital wi-fi in the new unit, as we had total control over the old unit, whereas new one required considerable input from the hospital IT department.
- It is essential to have a full-time research nurse during the data collection phase.
Professor Mark Tooley is a consultant clinical scientist, head of medical physics and bioengineering, and director of research and development at Royal United Hospital Bath. Dr Bernie Marden is a consultant neonatologist and lead paediatrician for the hospital. The research team also includes: Mike Osborne, Rebecca Abrey, Alex Reid, Debbie Grant, Lindsay Grant, Siu Man Lee, Sarah Mills, Emily Doe and Robert Eliot.



























No comments yet