The failure to meet the target for 95 per cent of all patients to be seen within four hours in A&E at acute trusts reveals patchy performance, but is it necessarily bad management, asks Robert Royce

Clock doctor
Arguably what the public expect above all else from an NHS accident and emergency department is to be seen quickly – within the national four-hour waiting time target in A&E – and admitted promptly, if required.
Unfortunately most hospitals struggle to do this on a routine basis. To be able to do so requires many things but above all:
- capacity for assessment in A&E and admission;
- adequate numbers of staff, preferably of a good quality; and
- an unremitting focus on waiting times and underlying processes.
This article analyses the last three years’ performance of 142 acute trusts against the target within the context of budgetary restraints and rising costs.
Management questions
If you work in one of the many trusts that have consistently struggled to hit the target, this can seem an impossible task.
However, its achievement is seen as the cornerstone of managerial “grip”; managers who fail to achieve this are deemed “bad” managers. We can examine the validity of that supposition by reviewing performance across England from 2011-12 to 2013-14.
This review looked at major, or type 1, attendances only because they are a better representation of A&E workload than “all types”, which include urgent care centres and walk in clinic patients.
Nationally reporting for all types typically adds about 2.5 per cent to performance. The three specialist children’s foundation trusts in England, which routinely operate at above 97 per cent, are also excluded.
Overall, England failed to deliver 95 per cent for type 1 attendances between 2011-12 and 2013-14. The fourth quarter of 2012-13 had the worst performance at 91.1 per cent. Performance dropped by 1.5 percentage points, from 94.92 per cent in 2011-12 to 93.42 per cent in 2013-14. Performance has subsequently improved but did not achieve 95 per cent in any quarter of 2013-14.
No firm foundation
Only 34 trusts (24 per cent) achieved 95 per cent in all three years. Of these, 26 were foundation trusts. The other eight have still not converted to foundation status. Of the 43 trusts that failed to hit 95 per cent in all three years, 23 had foundation status.
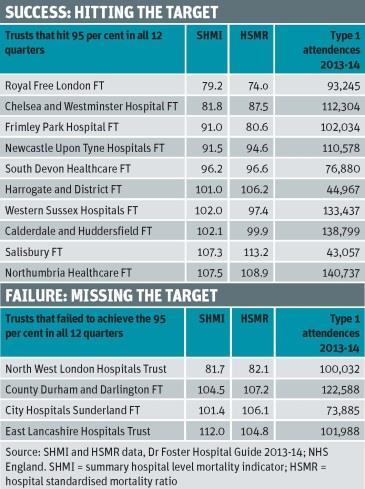
Only 10 non-specialist trusts attained 95 per cent in all 12 quarters. They were all foundation trusts: Chelsea and Westminster Hospital, Calderdale and Huddersfield, Salisbury, Newcastle Upon Tyne Hospitals, South Devon Healthcare, Royal Free London, Harrogate and District, Frimley Park Hospital, Northumbria Healthcare and Western Sussex Hospitals.
Four trusts failed to hit 95 per cent in any of the 12 quarters. These were: City Hospitals Sunderland and County Durham and Darlington foundation trusts; and East Lancashire Hospitals and North West London Hospitals trusts. If the cohort is expanded to include trusts that only hit 95 per cent in one of the 12 quarters, the number goes up to 19, five of which were foundation trusts.
The number of FTs that failed to hit 95 per cent has almost doubled in three years, from 26 in 2011-12 to 48 in 2013-14, out of 81 acute foundation trusts.
Geographical split
If you divide the country into the 25 local area team reporting areas, just two, Cumbria and West Yorkshire, achieved more than 95 per cent in the period. The local authority teams did not exist in 2011-12, but if they had only 17 would have exceeded 95 per cent. Only two achieved this in 2013-14.
Performance fell the furthest in Leicestershire, from 92.30 per cent to 88.34 per cent (3.96 percentage points). By contrast, the Surrey and Sussex area team actually improved by 1.4 percentage points from 91.62 per cent to 93.02 per cent.
Corporate activity may have affected the performance. The trusts that underwent merger or acquisition in the period – Lewisham and Greenwich Trust and King’s College Hospital, Hampshire Hospitals and York Teaching Hospital foundation trusts – showed some deterioration in performance.
‘The question as to what impact delays in admission have on mortality would benefit from more research’
Type 1 attendances rose by only 1.42 per cent in the three years but admissions from these attendances have gone up by 5.76 per cent. However, the link between four-hour performance and mortality rates was not as clear as expected.
Of the 13 trusts identified recently by health analytics firm Dr Foster to have higher than expected mortality rates, 10 failed four hours (many only just missing) in 2013-14.
However, Northumbria was on that list and it is also one of the 10 trusts that met or exceeded 95 per cent for the three years studied. North West London, which failed in all 12 quarters, has among the lowest hospital standardised mortality ratios and hospital level mortality indicator rates in the country.
Geography is density
The question as to what impact delays in admission have on mortality would benefit from more research.
The validity of the expectation that four hours delivery is achievable for all organisations, and failure to do so is “a failure of management”, can be questioned when 43 out of 142 acute trusts have failed to do so for three consecutive years.
Moreover, only 34 trusts achieved 95 per cent or more in all three years. Managers might be advised to take note of the old adage “geography is destiny”.
We might conclude from the above that for most places achieving the target is a constant struggle.
Relatively few trusts are in the equilibrium of either sustainable success, or continued failure. The deterioration in many FTs performance is also notable in this regard, particularly so given that these organisations were supposed to be well managed and well performing as a prerequisite of being granted “self-governing” status.
Common denominators
Unsurprisingly, all of the 10 trusts that hit or exceeded 95 per cent in all 12 quarters are FTs, but beyond that the similarities are hard to find.
Their sizes vary dramatically: Harrogate, Salisbury and South Devon have some of the smallest A&Es in the country, while Newcastle Upon Tyne and Chelsea and Westminster record more than 100,000 type 1 attendances a year.
Some trusts are single site, but others, such as Calderdale and Huddersfield and Western Sussex have two or more emergency departments.
Arguably, a number of these trusts fall squarely into the much maligned category of the “jobbing district general hospital” and several are unviable if the criteria that was used to assess Mid Staffordshire in terms of size and income were applied to them.
Given how much scrutiny this subject receives from commissioners, regulators and the likes of the emergency care intensive support team, more could be done to highlight what the successful hospitals have in common, and conversely, the chronic strugglers.
‘Both acute trusts and commissioners are generally focused on minimising four hour breaches to the point of obsession’
Over the period studied, the team has probably visited every trust at some point. They have accumulated and disseminated a large repository of knowledge about the management of emergency workload, much of it with a strong evidence base of what will normally assist a hospital to improve its performance.
Trusts do improve. Some, such as Surrey and Sussex Healthcare Trust, markedly so.
But many trusts have seen little, if any, improvement in performance in three years and the performance of larger number has deteriorated.
That deterioration is not marked, but the bottom line is that England’s performance has got worse each year since 2009-10.
Both acute trusts and commissioners are generally focused on minimising four hour breaches to the point of obsession. When that focus is linked to sufficient capacity this can deliver “good” performance, where “good” is primarily defined as hitting the target.
However, that does not necessarily mean that performance is good because of efficiency in the way that a factory returns a profit according to how efficiently it produces goods.
Arguably this is now the case with the NHS and the four hour target. An illustration of this is the “return” in terms of four hour performance that the additional £250m winter funding delivered.
Invisible inflation
At the same time, we are also seeing invisible inflation.
Invisible inflation is where you have all the conditions for inflation – high demand for a good or service that has limited supply, such as emergency doctors – but the authorities set a lower price than would be the case if it were left to the “market” to determine.
Several things can happen. The goods can disappear because nobody is prepared to sell them at the set price, or a black or alternative market arises where desired goods are exchanged at a higher price.
In the case of hospital A&Es, both are occurring. Junior doctors are voting with their feet, and a healthy industry has developed in providing locums at prices well above NHS salaries.
The same phenomenon has occurred in NHS management.
Hobson’s choice
It is very difficult to find people who want to undertake roles such as A&E manager or chief operating officer at the salaries on offer – or with the right skills and experience – and the interim market for such roles is correspondingly healthy.
The day rates charged reflect this. Costs rise, but the tariff reduces.
It is therefore little surprise to find large numbers of trusts in financial difficulties sitting across the spectrum of performance. Mid Yorkshire Hospitals Trust, for example, hit 95 per cent in 11 of the 12 quarters, but also has a multimillion pound deficit.
‘The fear is that missing the target leads to a near automatic label of being a “poor manager”’
Given Hobson’s choice between missing the money or missing the four hour target, many will see missing four hours as a surer route “to being moved on”, or worse. The fear is that missing the target leads to a near automatic label of being a “poor manager”.
More objectivity is needed. A starting point would be a greater focus on setting out the physical capacity and staff resources available at “successful” trusts to sit alongside the usual narrative about clinician engagement. Sitting alongside this should be transparency about the true costs of such delivery and a set of tariffs that reflect these.
We shall have to see if there is a turnaround in performance in 2014-15 and what it would take to make this happen.
Dr Robert Royce is an independent healthcare consultant
Topics
- Acute care
- CALDERDALE AND HUDDERSFIELD NHS FOUNDATION TRUST
- CHELSEA AND WESTMINSTER HOSPITAL NHS FOUNDATION TRUST
- CITY HOSPITALS SUNDERLAND NHS FOUNDATION TRUST
- COUNTY DURHAM AND DARLINGTON NHS FOUNDATION TRUST
- EAST LANCASHIRE HOSPITALS NHS TRUST
- Emergency care
- FRIMLEY HEALTH NHS FOUNDATION TRUST
- Government/DH policy
- HARROGATE AND DISTRICT NHS FOUNDATION TRUST
- Leadership
- London North West University Healthcare NHS Trust
- MID YORKSHIRE HOSPITALS NHS TRUST
- North East
- NORTHUMBRIA HEALTHCARE NHS FOUNDATION TRUST
- Performance
- Royal Free London NHS Foundation Trust
- SALISBURY NHS FOUNDATION TRUST
- SOUTH DEVON HEALTHCARE NHS FOUNDATION TRUST
- Targets
- THE NEWCASTLE UPON TYNE HOSPITALS NHS FOUNDATION TRUST
- WESTERN SUSSEX HOSPITALS NHS FOUNDATION TRUST
























6 Readers' comments