Heart sinking’ experiences of being called to crises for patients he had never seen have made Professor Michael Kirby an ardent advocate of health checks, reports Jennifer Trueland
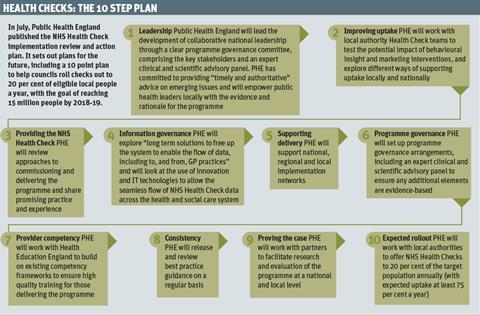
Health checks
To maximise benefits from the NHS Health Check programme, commissioners must look beyond the actual process itself, according to Professor Michael Kirby.
There’s little point in telling people that they have an elevated risk of stroke or developing diabetes if they aren’t then helped to make the changes to avoid the onset of disease or early death.
Likewise, public health teams will potentially be missing a trick if they do not ensure that the wealth of data generated from the Health Check process is not harvested and put to good use.
Professor Kirby, of the University of Hertfordshire’s Centre for Research in Primary and Community Care, has also been a GP for more than 30 years. He explains that the key is getting to the people in need, then ensuring there is proper follow through on whatever you find out. “As a GP I know that when you’re looking after a population of people, there are some people who come a lot, and some you never see.”
Warning signs
“You get a real heart sink feeling when you’re called out to see someone who has had a stroke or a heart attack and you’ve never seen them before. The signs of the risk were there, but they weren’t picked up.”
Rollout of the health checks so far has been “disappointing”, he says. “There hasn’t been a systematic approach. I think commissioners need to look at different approaches and not just assume that GPs will be the people to do this. GPs are flat out; they don’t have the resources and they don’t have the accommodation. What is needed is space and time.”
Making sure people are signposted to appropriate services or given the help to make necessary lifestyle changes is crucial, he says. This might include referrals to an exercise class, or a structured - or unstructured - series of “coaching” sessions.
Communicating risk in a way that patients understand is also important. “I’m a believer in giving people their ‘numbers’,” he adds, referring to the risk factors for various diseases. “That way they can take ownership of their health - you’re empowering them to make change.”
He explains the numbers are also hugely useful to commissioners of health services and to local authorities. For example, if a clinical commissioning group knows a certain number of people have pre-diabetes, it’s valuable intelligence when planning for how many diabetes specialists will be required.
Likewise, a local authority can use this information when deciding on priorities, such as building cycle lanes to encourage people to take exercise, or determining how many fast-food outlets or alcohol-selling venues there are in a given area.
Useful resource
Rosie Cunningham Thomas, chief executive of ToHealth, which has delivered more than 50,000 health checks across a variety of venues from shopping centres to public libraries, says the information they generate is an under-rated resource.
“When you look at our data, and you really drill down, it provides information at a really granular level, which helps commissioners understand the risk in their populations. For example, you might see that there is a particular risk with hard-drinking middle aged men in one particular housing estate, then you can use that information to do something about it.”
As well as providing information throughout a contract and at the end, ToHealth holds a “wrap-up” meeting to discuss the detailed findings and what they mean; often, she says, commissioners are astonished by what they find.
“I’ve had people say to me that they knew they had a problem, but they didn’t know it was that bad,” she says. “The really switched-on commissioners are the ones who get it - and plan services accordingly.”
She cites one commissioner who set up a weight-loss programme for young south Asian women as a direct result of information received from checks performed locally.
She believes the NHS Health Check programme is just the starting point for a holistic, preventative approach to health and wellbeing - and that if it is to work, you have to close the loop between the check, the patient’s GP and follow-up care. “Really good data is vital, because then you can bring in analytics, and really begin to close the loop,” she says.
Using data better
Katie Hall, chair of the Local Government Association’s Community Wellbeing Board, says local authorities are alive to the possibilities brought by the NHS Health Check programme data.
“It is crucial that health and wellbeing boards use the information from NHS Health Check, especially data on the risk of developing preventable conditions and the inequalities between different communities to inform their joint strategic needs assessments and joint health and wellbeing strategies,” she says.
“By bringing NHS Health Check into the commissioning strategies of local authorities, they will be able to join up with wider local authority services such as family support, education, culture and housing.”
She says there are four key factors which would ensure that full benefit can be realised from health checks and the data which flows from the programme. First, ensuring variability of health check uptake and information on risk factor data is systematically embedded in the joint strategic needs assessment; second, ensuring that where there are significant differences in uptake, these are addressed in the recommissioning of contracts; third, ensuring best value is achieved by exploring a range of existing and potential providers; and fourth, ensuring the quality of Health Check so that everyone who needs further information, support and treatment is referred to the most appropriate source, whether this is via further diagnostic services, public health or access to leisure facilities.
Ms Cunningham Thomas believes people should be enabled to take control of their own health, and says innovation through technology is a key part of this.
Self-management
Increasingly, technology is helping people to self manage long term conditions and with more and more people owning smartphones and tablets, this is only expected to become more important.
“With smartphone penetration so high you don’t even have to provide the hardware − people have already got it,” Ms Cunningham Thomas says. “Innovation through technology is key to prevention and helping people self-manage − and health checks are just the starting point.”
Critical point for checks − an HSJ/LGC supplement
How to increase the uptake of NHS Health Check
- 1
- 2
 Currently
reading
Currently
reading
'The signs were there, but weren't picked up'
































No comments yet